Miracle Mateo
I truly believe in miracles because of our son
Today is our son Mateo’s second birthday. As I reflect on him turning two, all I can think about is the concept of miracles.
According to surveys, 70% - 80% of Americans believe miracles are real. I would definitely be one of them. But belief is a funny thing. While I believed in the concept, that miraculous things happen in the world. If you asked me to point to miracles in my own life, I would hesitate. Not because I haven’t had wonderful, unexpected things happen. I’m just not sure anything ever felt like it met the full definition.
In the Catholic Church, a miracle is defined as:
an extraordinary event, such as a healing or control of nature, that is impossible to explain by natural causes and is considered a direct sign of divine power.
“Extraordinary.” “Divine.” These are incredibly strong words that didn’t seem to fit any particular event in my own life.
This all changed when our son Mateo was born.
Becoming a parent gives you a great appreciation for the amazingness of life emerging right in front of you. Now, when I see someone having a child, I think, wow, what a blessing. It’s such an amazing thing, I really wouldn’t disagree if anyone called their child a miracle. But when I think of Mateo, when anyone asks me about him, the *very first* word I think of is: miracle. As he turns two today, I sit here and reflect on what a miracle he really is.
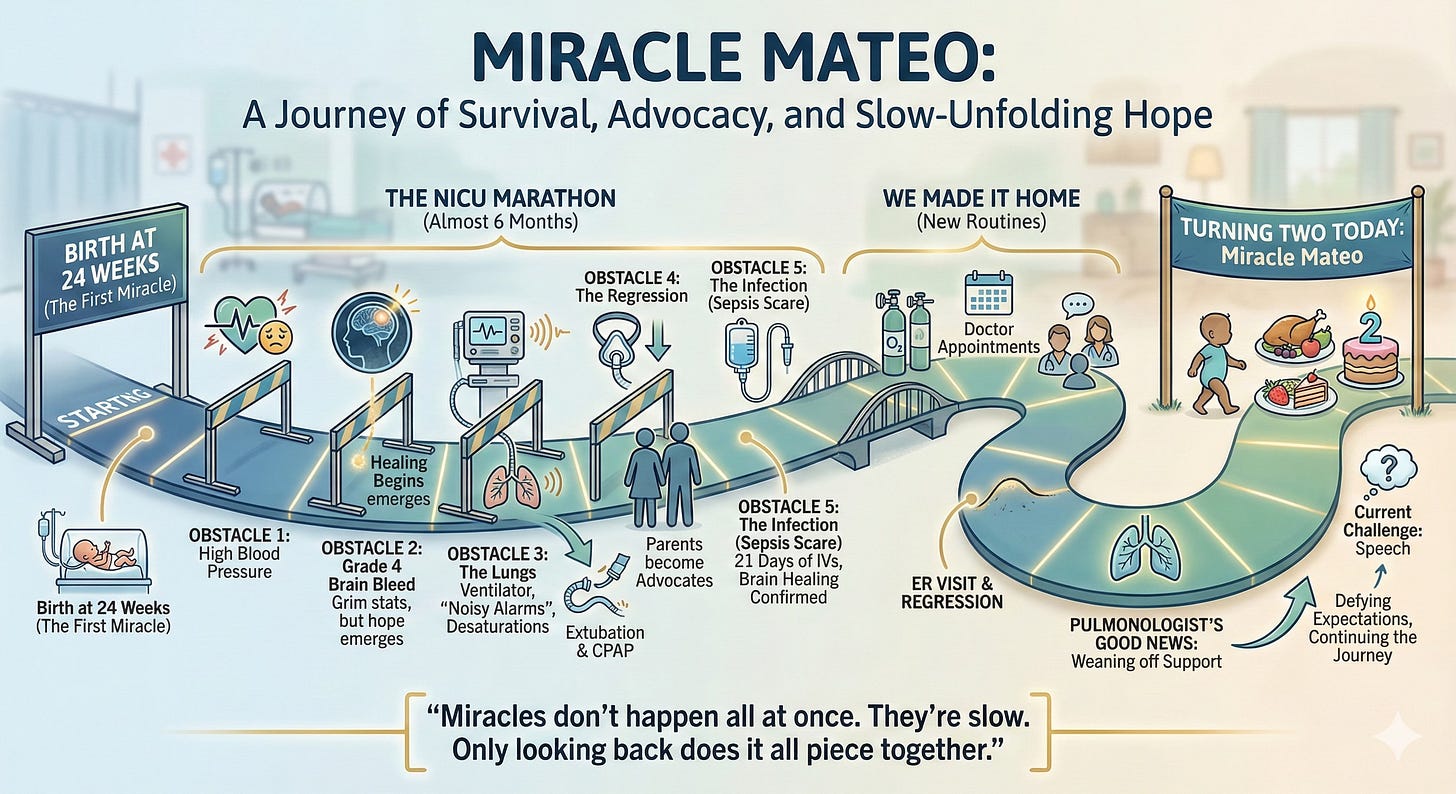
Mateo’s birth was a miracle in itself, at 24 weeks. I talk about it here. Months after he was born, I remember reading about his “medical case” in the hospital. It said he needed two separate sets of chest compressions (+ epinephrine) to keep his heart beating. Surfactant to open up the lungs. A ventilator to breathe. The fact that he even made it out of the surgery room was our first miracle. Up next was being sent to the highest level (level-4) neonatal intensive care unit (NICU).
During our almost six months in the NICU, it felt like everything was against him.
Obstacle 1: The Blood Pressure
First, the steroids for his lungs weren’t helping. Then, as they started to work, he developed concerningly high blood pressure. Every day we watched that number on the monitor. We stressed as the attending doctor walked over and asked the nurse what his blood pressures were.
If I were to describe the NICU journey, it felt like a marathon race with multiple distinct legs. Like a spartan race, with different obstacles at each leg. But it wasn’t a race, it was more like survivor. The goal was to just make it through to the next obstacle. If each major challenge was an obstacle, the first one was his blood pressure. We did not know it at the time, but this was a tiny challenge compared to what was to come.
Obstacle 2: The Brain Bleed
Next, we heard about his grade 4 brain bleed, the worst level you can have. The statistics are grim: about 25-40% of babies don’t survive, and for those that do, there is a high risk of cerebral palsy and major cognitive delays. We were told kids with grade 4 bleeds had as high as a 50/50 shot of cerebral palsy. Everything I read online seemed to back up the grim prognosis.
Around this time, his breathing started getting worse. They switched him to a more intense ventilator. For weeks when we were by his side, or when we would call in, the updates weren’t good. He wasn’t decreasing his ventilator support, which became the new, most important goal.
Obstacle 3: The Lungs
We quickly learned his lungs were sick, very sick. We were told he had the premie version of chronic lung disease. I would sit by his bedside and read about the prognosis. One quick conclusion I gathered was how ventilators provide a child with life, but damage their lungs at the same time. Basically, the longer he was on a ventilator, the worse his long-term outcomes. What if he never got off of it? I thought to myself. After driving to the hospital one Friday night, we called in and got another bad update from the nurse. “He had many ‘events’ today, and needed to receive manual breaths more than once”, the nurse said. It was a nurse we never had and she sounded indifferent (which was rare). My wife and I were upset and frustrated. “Let’s talk to the doctor”, I said. We asked for the attending physician to come to talk to us when we arrived. All that I remember about this conversation is that it was not encouraging. The doctor explained to us that he needed time to grow his sick lungs, and it was too early to assess. But he did not want to give us false hope.
“He could be on a trach someday where a machine breathes for him, but we don’t want to worry about that now.”, the doctor explained.
How could I not worry? We tried to keep hope, but it was beginning to feel hopeless.
He was on so many pain meds it was hard to keep track. He wasn’t very alert. There was not much we could do but sit there and hope. I prayed. We went to mass and continued to pray. Our priest drove an hour to come see him. We were hoping for a miracle.
But nothing seemed to change. At one point Mateo pulled the ventilator tube out of his body and had to be given manual breaths. It was scary moment after scary moment.
When I think back to this period, I think about his horrible desaturation “episodes”. We’d sit there and he would be breathing normally and all of a sudden you’d hear an alert. His blood oxygen would shoot down below 80, below 70, and the alerts would get louder and louder. The nurse would look stressed. We had multiple weeks like this. If we heard alerts go off in the room, we knew it was Mateo. Every 15-20 minutes, a severe alert. I felt like I was in a high-stress movie. Hours of that experience. Every 30 minutes the alert would go off and I’d think, here we go again.
The nurses would almost joke about him being the “noisy” one in the room. In a room full of sick babies, if you heard a beep, you knew it was Mateo. I smiled along with them, but inside I was gutted.
At that time, the one thing giving us hope was his “eating”. That just meant when they pushed milk into his stomach via a g-tube, his body was not rejecting it. We learned this was important because the lungs needed to grow healthy tissue. The hope was that as he gained weight, he would grow healthier lungs to help overcome his diseased tissue. As he grew healthier lungs, he could lower his ventilator support. Our new scoreboard became what his oxygen level for his ventilator was. “Room air” was 21%, meaning the ventilator was not providing him any oxygen. The ventilator could get close to 100% meaning the air pushed into his lungs was maximum oxygen. He was usually between 40-50%. We would call in as soon as we woke up to check how he did over night. “What’s his oxygen at?”, we would ask. Hoping to hear a lower number. For weeks, it felt like every time we called, his number would only be worse. Or, they would try adjusting a different setting to increase his breathing support.
But as he gained weight, and the steroids kicked in, we hoped to see movement in the right direction over the coming weeks. This was what happened. His oxygen support lessened slowly each day. We were now close to two months since he was born.
The night before they pulled the ventilator out was actually horrible. I remember as we were driving to the hospital. We called, and they told us that the attending doctor switched his ventilator mode. He seemed to like it. They said he was doing better. His lungs seem to work better with the new mode.
Later that night, another doctor came in and switched his ventilator mode back. I was frustrated, but her explanation made sense. She calmly explained to us that the new mode could lead to a collapsed lung, and she wanted to avoid that. But he clearly hated it. His heart rate was flying up. It got so bad, a nurse put cold water on him to try to slow it down.
The next day, the first doctor was so fed up by the debate of which mode to do, that she thought it was time to take his tube out and give him a chance to breathe on his own. Looking back, it’s interesting how something that seemed like such a bad thing (switching modes) may have actually worked out in our favor.
It was two months since he was born and they went for it. They pulled out his ventilator and he was given the chance to breathe on his own (with CPAP air in his nose). They told us not to get too excited because he might have to go right back. They said babies all the time have to go back on a ventilator because their lungs get tired out, or they just become dependent on having a machine breathe for them.
Thank God he never had to back to a ventilator again. Our little guy fought like hell. And he was doing it.
It was a miracle. But here’s the thing about miracles, at least the ones we experienced. They don’t happen all at once. They’re not a single moment. They’re slow. As it was happening, you couldn’t see it. Only looking back does it all piece together.
Obstacle 4: The Regression (Lungs Pt 2)
For weeks, we walked in each day and I took a deep breath of relief when I saw the CPAP machine. Each day was another day he was off the ventilator. I felt like the longer he was away from the ventilator, the less of a chance he would ever have to go back on it.
Weeks later, as Mateo seemed to be stable, I remember going home to be with our cats for a few days. On my third day at home, my wife had been texting me concerned. “He’s not doing well”, she texted me. At the time, I didn’t make much of a deal about it. I figured as he’d been going weeks with breathing well, this had to just be a bad day or something. He has already lowered “his pressures”, on his CPAP. This was our new scoreboard. For the prior few weeks, we would get positive updates every few days. “They (the doctors) decided to move him to CPAP-4”, the nurse would tell us. As he moved from 6 to 5 to 4, we were getting closer to our next goal, to get to a continuous flow (high flow) of air in his nose.
Later that night, my wife called me, extremely concerned. “He’s not doing well at all. You have to get up here. Something’s wrong.” “I don’t understand, he’s lowered his pressures for weeks”, I said. My wife said they had raised his pressures multiple times in the last few days. His lungs seemed to be regressing.
When I arrived it was worse than expected. Mateo couldn’t keep his blood oxygen up. He just wasn’t the same guy. He looked the same, but his alerts were happening again. The doctor made his CPAP machine stronger. He was on max support. The oxygen pressure was so high you could feel it in his back being pumped in. If he continued to struggle, it meant only one thing: back on a ventilator.
I didn’t understand what happened. We cried in the waiting room in the hospital. Was it the new food they put him on? Was it the fact that they were obsessed with putting him on his back all of a sudden even though it’s harder to oxygenate on your back? Whatever hope we had felt distant at that moment.
We went back to Ronald McDonald House worried we would walk in and he would be back on a ventilator in the morning. We worried. We prayed.
We walked in the next morning and he was still on his CPAP. We were now months into the NICU and were comfortable advocating for him. One of our favorite early nurses told us invaluable advice in the first two weeks there. “Your most important job is to advocate for him. He can’t for himself”. We took that to heart. But at first it is difficult. You trust the providers and you don’t want to make people angry. Especially as we were going to be there for months. But after 3 months there, we were comfortable and we had been learning as much as we could, day in and day out. If there was one thing I could do, it was read everything I could about Mateo’s situation.
We pushed nurses to lower his support when he was doing well. We fought with nurses and doctors about letting him sleep on his belly, where he was safe and oxygenated better. We got him on a new formula which. supplemented his breast milk (we later found out he had a cows milk allergy which might have explained some of it). We wanted to have no regrets that we didn’t do everything we could.
My wife and I had a mental switch around that time. We weren’t just observers anymore; we were going to fight along side him. We were there at every single weekly doctors rounds, which were usually around 9am. We waited until the attending doctor got to Mateo’s bed side to give the report to the medical students. They begin to notice and would walk over to us, prepared to give an update. If Mateo was going to fight like hell, so were we. I think we started to frustrate some of the nurses or doctors, by being there 24/7. Some loved us, some did not. We did not care. My wife decided she wasn’t going home until Mateo was. It was now close to 3 months in.
Day after day, he was still on his CPAP. And slowly, his numbers got better. I’m not sure if what made the difference, but he fought every day, and once again they started to lower his respiratory support.
Miracle Mateo kept fighting.
Obstacle 5: The Infection
Another month later, things were going pretty well. Then one night we were excited because that day we could try a bottle for the first time. Until then he had only gotten food through a tube directly to his stomach. We took pictures with him getting his first bottle. That night, he was breathing fast. I thought it was just because he had so many new things happening.
That night we got a call. He had a serious infection and was going into sepsis. Sepsis is one of the top concerns for micro-preemies, with a mortality rate around 18%, and even higher for certain types of infections. Luckily they caught it early enough to put him on antibiotics. After multiple failed spinal taps, none of the tests were conclusive about what type of infection he had. They had to do 21 days of IVs. He would pull out the tubes almost every day, making it hard to find a new spot.
This new setback nearly broke my wife. She was so fed up of almost being out of the NICU, that things were going well, but now he got an infection. We later found out he somehow got E. coli. Thank God they caught it. If the doctor that night did not make the aggressive call to start antibiotics immediately before results came in, he may not be here today.
He continued to progress and grow, despite dealing with the IV in his arm that he hated and tried to pull out constantly. We made it to the end of this 21 day treatment and moved to the part of the hospital with the least sick kids.
Miracle Mateo.
Around that time, one of the doctors walked into the room. “Hello, Acton family,” she said. “I have to show you something.” She was one of the longest-tenured doctors in the NICU, and she had this glow on her face. She was excited. She walked us through the pictures of his brain—the original ultrasound, then each one after. You could see the ventricle getting better, image by image. She was so elated to show us. Then she said something I’ll never forget:
“I don’t like to use the word miracle or get your hopes up too much, but this is about the closest to a miracle as you’ll see regarding his brain healing.”
The biggest challenge he had going forward was his brain. And we were watching it heal.
We made it home
We had finally made it home. We transitioned to the new challenge of having, not just a new born at home, but a micropremie with chronic lung disease. Doctors appointments every week. Hours in the car. Specialists in every area had to see Mateo. Weekly deliveries of oxygen tanks for Mateo. At home therapy visits. Physical therapist. Occupational therapist. Speech/food therapist. Stomach meds in the morning. Breathing treatments three times a day. These became our new routines.
We had small good news along the way. His brain development looked good so far. No seizures during an EEG. The gastrointestinal doctor prescribed us a high quality formula and stomach meds. His digestion improved.
Being a first time parent of a micropremie at home, you are sort of learning two new things. First, like other first time parents, we were just learning how to take care of a baby. Second, we were learning how to be a medical care team for a sick baby. Now that we have two babies, I can say *it is not the same* when you have a micro premie at home. One of us always had to be awake with him early on. We did shifts for sleeping to make sure his oxygen levels were good and his tank wasn’t running low.
It was a lot of work. Luckily, for us, it was the summer, and my wife and I are both academics. We were making it. Mateo seemed to be breathing better. We felt optimistic things would only continue to get better and we could get him off oxygen support.
The obstacles, and miracles, continue
After being home for a month and doing well, we noticed his breathing wasn’t as good. He wasn’t sick, but he was struggling to keep his blood oxygen above 95%. We called our pediatrician. They said go to the hospital. We didn’t understand — what had happened? He wasn’t sick. He was doing so well the week prior. Did we do something wrong? That familiar pit in our stomachs from the NICU returned.
The ER was incredibly stressful. Six hours before we got a room. No clear explanation. Was this another regression? We feared the worst. After a couple nights, his breathing was stable enough to come home, but with higher respiratory support than before. It felt like a punch in the gut. We hoped for another little miracle. We prayed for improvements. Would it always be like this? Would he always need oxygen support because his lungs were so sick?
The next week we stayed focused on him. We did everything we were told to do. Over time, he was breathing better. We learned small details about how we could make his breathing treatments more effective. We stayed patient. Another month went by and we finally had his important doctors appointment an hour away — the pulmonologist. This was a specialist for Mateo’s most critical area, his lungs.
We probably didn’t hear more positive things about any doctor than we did about his pulmonologist. “You will love him”, one of our NICU doctors told us. We were anxious and excited for this visit. We had to wait months because he was so busy.
It was the day of his appointment, and we were feeling hopeful. Mateo had a really good month since his hospital visit breathing wise. The little guy was making improvements every day on his oxygen levels. We were hoping the doctor would say his lungs were doing well, but we weren’t sure.
When the doctor walked into the office, it quickly became clear how right everyone was about him. Smart and kind, he sat with us to answer any questions we had, and we had a lot. “I’m sorry, it took so long for me to meet you all”, he said, with a truly caring look in his eyes. He continued, “But I have great news”.
“Mateo is one of the best looking 24 weekers with his case history I have ever seen at this point”.
He continued that we could start doing trial runs with zero breathing support, and once he passed the overnight breathing test, he could move to zero oxygen support. We were elated.
After being told that he may never be able to breathe on his own. That he may be tethered to a machine. After being told that he had some of the sickest lungs in the NICU (out of hundreds of babies), he was going to be breathing without any support. Looking back at these moments, I think of only one word: Miracle. During the next checkup, the pulmonologist said his overnight breathing test was the best he’d maybe ever seen in his career for a micro-preemie.
Over the next few months, we gradually weaned all of his medications. No more breathing regressions. He even got sick with a cold and his breathing did not get worse. He was now a kid that didn’t need any daily respiratory medications.
Miracle Mateo.
When he could finally start trying foods, he would constantly choke on them. He would throw up all the time. He just struggled with food. Today, while he doesn’t want to eat many foods like a lot of kids, and we still have to be careful with choking, I’m amazed to say he eats so many different things, fruits, veggies, chicken, hamburger, pineapple, cake. This was a kid who literally wouldn’t eat one piece of food without throwing up. That kid who was on tubes to his stomach for months is now eating all this.
He was clearly behind in physical movement. He couldn’t roll over. He couldn’t crawl. He was past one year old. He seemed extremely far away from walking. But as time went by, he started to amaze us. Six months later he was walking. Already learning complex things like stairs.
When he started physical therapy, his PT said he was at the first percentile for kids his age. Now, today, she said he tested close to the 40th percentile. Almost average. He can kick a soccer ball. He can go up steep stairs with a railing. He can almost throw a ball.
This is Miracle Mateo.
Now that he’s two, his current challenge is speech. He’s behind, and we’re working on it. But the thing I keep telling myself is that he’s broken every other expectation set for him. He’s been a miracle at every step of the way. Why wouldn’t he continue?
These days, he goes to daycare. He’s around “normal” kids. To everyone else, he’s just another two-year-old. And we take it for granted sometimes, how ordinary his life has become. But if I could go back and tell myself in that NICU, watching the monitors and listening for alarms, that Mateo would be where he is today? I would have said: that’s incredible.
That’s the thing about some miracles. You can’t see them while they’re happening. You’re too busy surviving. It’s only now, looking back, that I can see how it all pieced together.
So today I celebrate our wonderful Miracle Mateo turning two. If someone asks me if I believe in miracles, I’ll tell them about my son.
Happy birthday, Miracle Mateo.


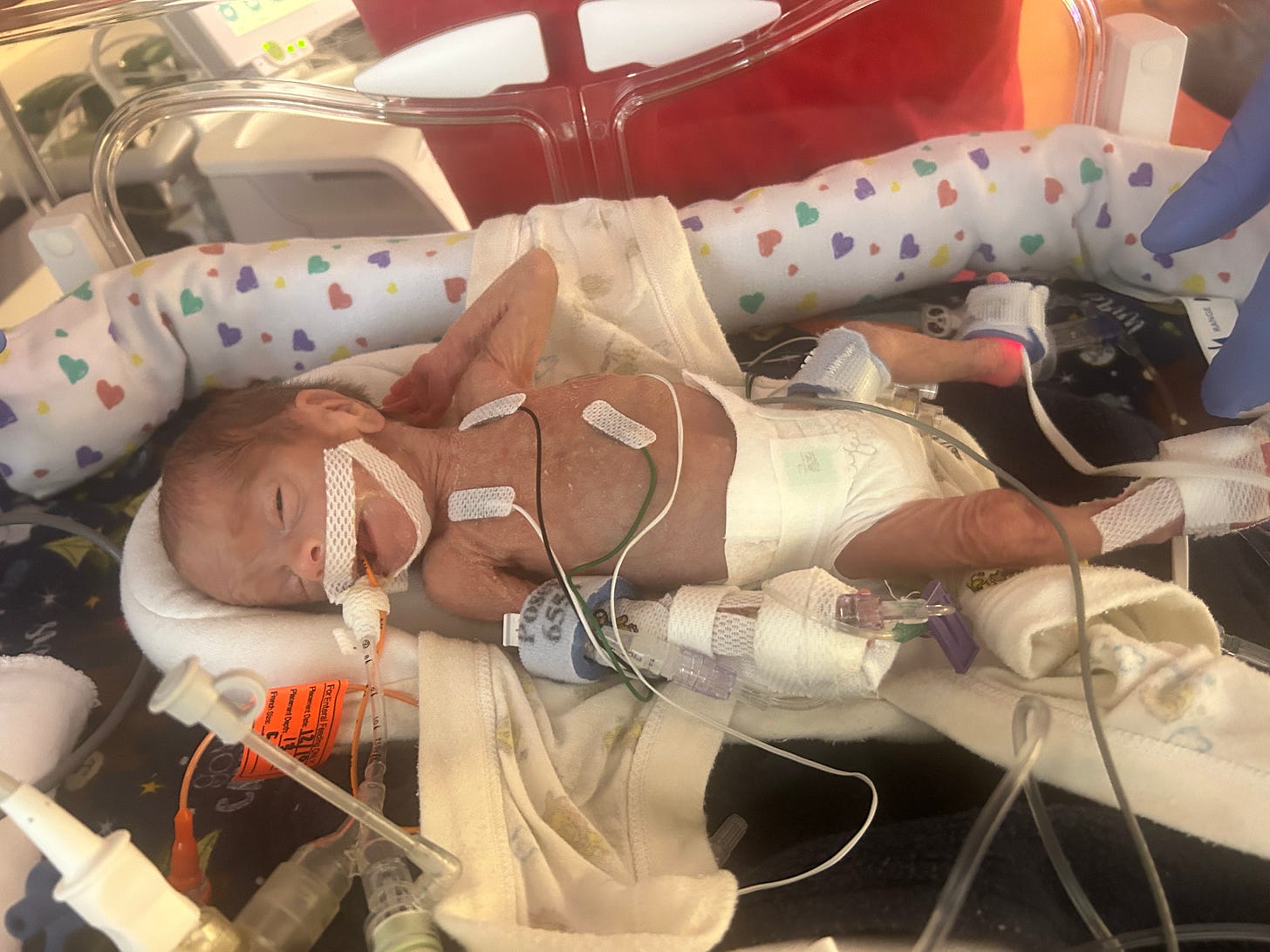
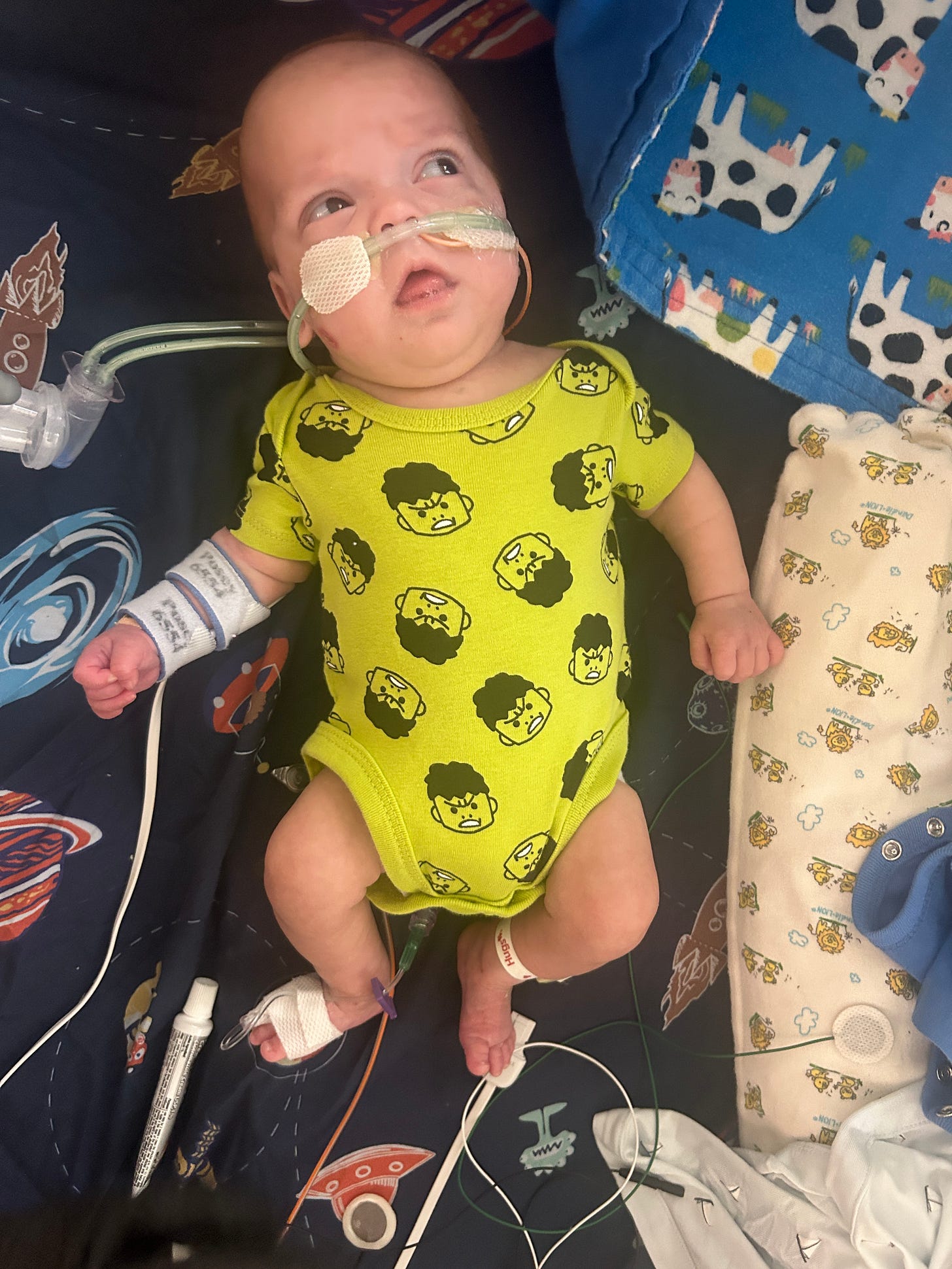
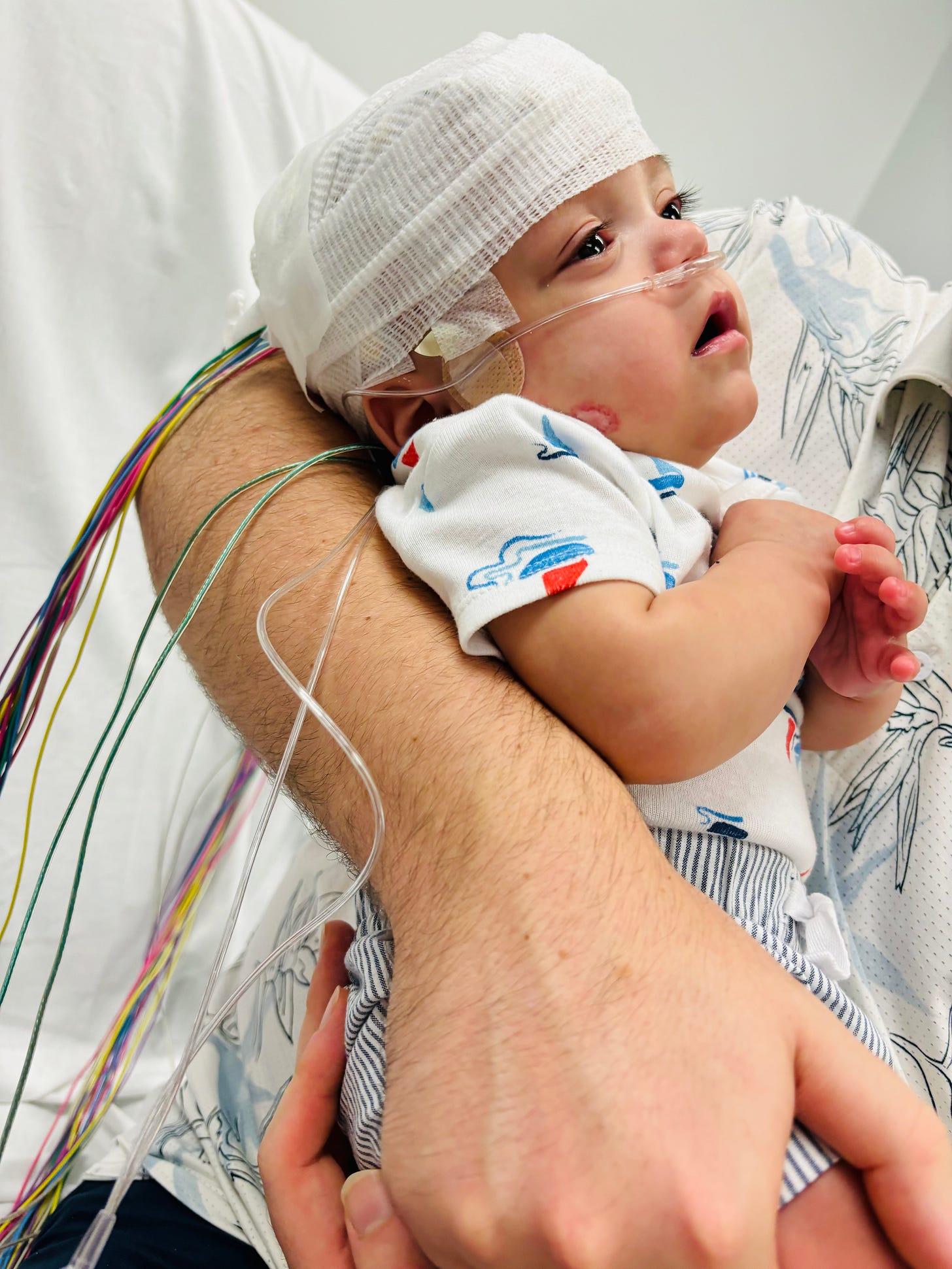



this is a beautiful story and as someone who went through something similar with my son this year, it fills me with hope that there are people like you who are giving parents who are currently in the NICU that same hope we needed while we were there.
You really nailed it with the anxious feelings that all parents feel when they hear a bell or a desat on their baby in the room, I got flashbacks to when we would see desats and it is never fun but I look back at that time in a strangely fond way. He wouldn't be here without that time and being parents of micro-premies makes you really appreciate all the things they have to fight to achieve.
I am excited to see Miracle Mateo grow up! The world has no idea whaggha fighter it's going to see.